Within the wide array of tissue types in the human body, each has its own specificity based on the purpose and function it provides. Muscle contracts and expands and enables movement of and within the body. Epithelial covers the body surfaces and lines internal cavities and vessels. Nervous tissue transmits impulses and stimulates bodily functions. Connective tissue provides structure and support of the body and the organs within. All three formerly mentioned tissues are of a soft-tissue nature. However, the last category is unique in the density and fibrous nature of cells more than any other type, which further differentiates into hard-tissue or bone.
While blood and lymphatic tissue surprisingly fall into the same category, the specificity of cartilage and bone provide unique challenges for the Histotechnologist and commonly require special treatments to render the tissue diagnosable. Bone tissue can be said to be the most challenging tissue to prepare, mainly because of its cement-like nature. While bone may have the appearance of being rigid inactive tissue, it is in essence living tissue that has formed from a dense matrix of collagen and mineralized protein. Osteoblasts are the bone forming cells that secrete a substance called osteoid.
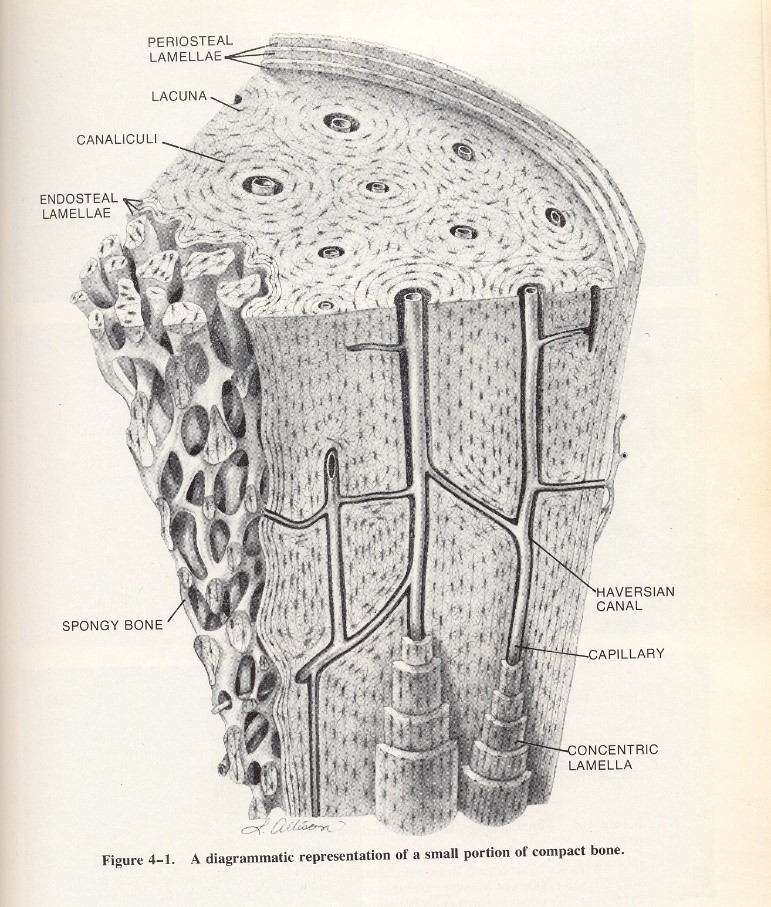
Inorganic salts of calcium phosphate are deposited by the osteoblasts and mineralize into the cement-like matrix. The osteoblasts become trapped within the matrix and differentiate into osteocytes with a visible, living nuclei that can be seen microscopically in spaces called lacunae. Osteoblasts in the tissue continue to form new bone matrix as the bone continues to grow and replace old cells.
Bone forms into circular columns of concentric lamellae that surround what is known as the Haversian canal system. The Haversian canals are the primary vascular system within bone that allow blood vessels and nerves to travel through and nourish the bone. Branching passages called canaliculi allow nutrients to be passed to osteocytes and provide for the elimination of waste products within the tissue. A close look at the internal anatomy of compact bone above demonstrates the living nature of bone as it continually grows new cells, provides blood and nourishment for existing cells, and replaces older cells called by reabsorption of bone.
In cases of pathology such as degenerative bone disease, it is necessary for the pathologist to take a detailed look at the normal/abnormal morphology of the bone specimen. As previously mentioned this presents a challenge to the Histotechnologist because the dense nature of the specimen. It does not allow sectioning to be done through routine microtomy. Laboratorians must first use methods to break down the calcium salts in the specimen rendering it flexible and pliable enough for the microtome blade to smoothly pass through the tissues at 4-5 microns thickness. Technologists typically use a process of breaking down the mineral salts using acids and/or chelating agents. The acid can be a strong acid such as hydrochloric acid, or a weaker acid such as formic acid. One of the most common chelating agents is EDTA. Oftentimes a decalcifying solution will have a mixture of acid and chelating agent to allow the technologist to have greater control over the process and not over decalcify the tissue. Pathologists need to be able to view the discrete nuclear detail of the tissue, and prolonged or extended decalcification past the end-point will deplete the nuclei of all basophilic properties and not stain with hematoxylin.
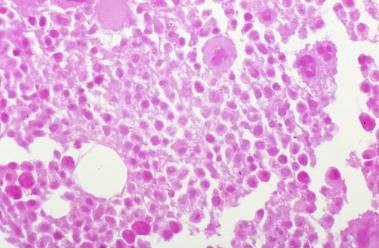
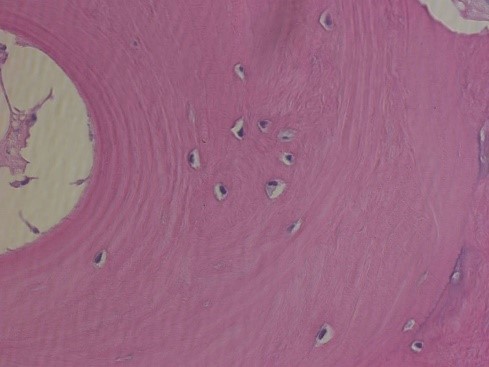
So, in essence, decalcification must be monitored closely and ended at an optimal time. Note the image to the left showing over-decalcification of a bone marrow specimen. There are no visible nuclei left in the tissue because of the over exposure to decalcifying acids. Contrast this with the image on the right of another bone marrow specimen with optimal decalcification. Note the nuclear staining within the osteocytes as they sit within their lacunae spaces. Also note in the image on the right the concentric lamellae rings showing the continuing deposit of bone materials by the osteoblasts.
Lab Storage Systems has the products and solutions to ensure your success in the laboratory. For information on products, techniques, and troubleshooting, contact our Technical Marketing Specialist today.
References:
Allison, L., Graphic images in bone anatomy, Adopted in LMC Development Curriculum-Anatomy of Bone & Principles of Decalcification, 1996.
Brown, S., ‘Fundamentals in Microwave Decalcification’, Microwave protocol development, Lab Management Consultants, 1998.
